Vitreous pathologies: an often misunderstood problem
In the field of Clinical ophthalmology A problem that is very often overlooked or underestimated, but which creates considerable discomfort for those who suffer from it, is becoming increasingly widespread. We are talking about vitreal pathologies: a series of pathological changes affecting the vitreous body causing significant visual discomfort, especially under certain lighting conditions.
More and more often, in fact, we are faced with diagnoses of vitreous turbidity, syneresis, vitreous detachment e synchysiswhich most often go untreated or, worse still, minimise the symptoms that remain a major problem for sufferers.
These symptoms in many cases have a negative impact on the emotionality and serenity of the patient who is faced with a problem that he or she has to live with, without any hope of finding a solution.
In recent years, however, technological evolution, which has led to the development of the minimally invasive surgeryallows one to address and, in some cases, eliminate the vitreous alterations thanks to therapeutic and surgical actions aimed at adequately treating the specific clinical case.
We can therefore state that the patient with vitreous disease can currently hope to eliminate the discomfort related to vitreous opacities and does not have to learn to live with the problem but, if properly advised by their ophthalmologist, can choose the best solution that best meets their expectations.
The vitreous body: what is it?
Today we know that the vitreous body, or vitreous gelIt consists of transparent, gelatinous connective tissue that is neither vascularised nor innervated. Weighing approximately 4 grams, it makes up two-thirds of the entire eyeball volume and, due to its size, contributes to the shape and substance of the eyeball.eye.
Due to its high viscosity, the vitreous acts as a shock absorber for possible bulbar trauma, protecting the most delicate ocular structures. In addition to these numerous properties, its elasticity allows antero-posterior displacements of the crystalline lens, helping the ciliary muscle in its accommodative activity.
The vitreal gel consists of 99% water and the remaining 1% collagen fibrils and hyaluronate, which form the 'scaffold'. The network of collagen fibrils forms a solid structure that is 'swelled' by the hydrophilic hyaluronate, creating the actual vitreal structure.
The relationship between these two elements is crucial to maintaining the transparency and structure of the vitreous, as if the proportions between the two were to change (such as during ageing), the vitreous would become more liquid and less 'gel-like'.
Fibrils consist of type I and type II collagen with a triple helix structure.
Lo vitreal development begins during the sixth week of embryonic life and, although the origin of cell development is not yet entirely clear, it is assumed that vitreous synthesis is due to hyalocytes, retinal cells and ciliary body cells.
During theembryogenesis The vitreous is invaded by blood vessels, which provide nourishment to the developing anterior segment of the eye. Over time, these vessels regress until they disappear completely, leaving the vitreous body transparent.
Its volume increases threefold from birth to adulthood; however, it should be noted that 70% of this increase occurs by the age of four. Complete development is generally reached in the adolescent period, between 15 and 18 years of age.
The formation of the vitreous gel consists of three different moments that contribute to the composition of the final vitreous:
- Primary vitreous: mesodermal tissue surrounds the lenticular vesicle, while in its inner thickness, a vascular web from the hyaloid artery develops.
- Secondary vitreous: It usually forms around the second month of intrauterine life, through a process of transformation of mesenchymal tissue with typically avascular neuroectodermal tissue.
- Tertiary vitreous: characterised by the disappearance of the hyaloid vascular tree and consequently the appearance of the Cloquet Canal. This portion of the vitreous represents a virtual cavity and is optically empty, composed of the primordial mesenchymal tissue now replaced by the definitive vitreous.
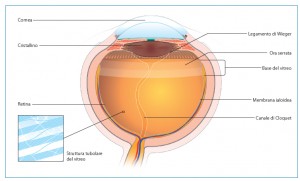
Anatomically speaking, the vitreous body is usually subdivided into three different well-defined zones that are called: Central Vitreous, Vitreous Base and Vitreous Cortex.
The Central Vitreous is, as its name suggests, the portion in the centre of the entire vitreous gel which contains within it the Cloquet Canal, which is a remnant of the primary vitreous vascular system during embryonic development. The central vitreous has a low concentration of collagen fibres running antero-posteriorly.
The Vitreous Base is located at the ora serrata, the transition portion between the retinal tissue and the ciliary body. In this anatomical area, the vitreous is characterised by the presence of dense bundles of collagen fibres strongly adhered to the retina, probably due to their 'fusion' with the inner limiting membrane.
Vitreous cortex: the central vitreous gel is in turn surrounded by the vitreous cortex, which has a different orientation of collagen fibres than the central vitreous. The cortex is commonly subdivided into:
- Anterior vitreous cortex: covers the posterior surface of the lens at the patellar fossa.
- Posterior vitreous cortex: this vitreal portion adheres to the innermost retinal surface behind the posterior edge of the vitreous base.
Vitreous diseases: how can we prevent them?
To carry out a simple but effective prevention of degenerative vitreous diseases The patient should always be reminded to take a significant amount of fluids, especially in summer, in order to counteract water loss due to diuresis and perspiration.
In the presence of overt vitreous degeneration, simple rehydration of the vitreous gel, preferably enriched with osmotic substances, favours the re-expansion of the vitreous mass and reduces the movement of the broken fibrils within the vitreous lacunae, allowing a marked decrease in the perception of mobile bodies, with a clear improvement in subjective phenomenology.
Unfortunately, dietary administration of hyaluronic acid and collagen does not result in vitreous accumulation, due to the immediate degradation of these molecules by the stomach's gastric juices.
Indeed, the degradation of vitreous fibrillar matrices is due not only to natural enzymatic mechanisms and the action of free radicals, but also to the effect of certain classes of drugs used in general medicine.
For example, in hypertensive patients or diabetics in chronic treatment with antihypertensives and diuretics, the constant depletion of water and potassium tends to reduce the aqueous component of the vitreous mass and consequently to alter the correct ratio between this and the fibrous component, as well as to favour vitreoretinal traction.
The main vitreous pathologies
Haemovitreo
This is a haemorrhagic clouding of the vitreous body, resulting in blood mixing with the vitreous gel and the formation of masses that are not very transparent or not at all, which can significantly impair visual function.
L'haemvitreous can be due to trauma of the eyeball or, more simply, it can occur spontaneously. The main causes of spontaneous haemvitreous can be diabetes, arterial hypertension, retinal vascular diseases, retinal ruptures and subretinal neovascular membranes.
Hyalosis Asteroid
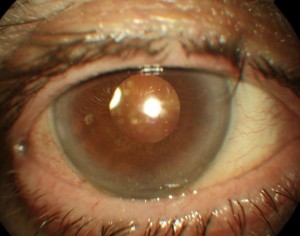
The hyalosis asteroid is a rare condition that is generally found in individuals over the age of 60 and is more common in diabetics. It corresponds to an ageing process of the vitreal collagen.
The characteristic appearance of asteroid vitreopathy is represented by the presence of shiny, yellowish-white round opacities (asteroid bodies) suspended in the vitreous gel, often aggregated in clusters and looking like strings or clusters of pearls.
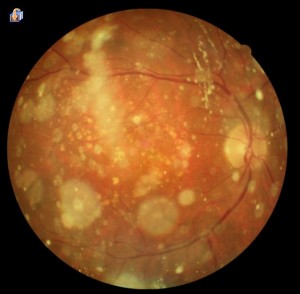
The asteroid bodies, composed mainly of fat and calcium salts, are attached to collagen fibres and are mobile with the movements of the vitreous gel.
The asteroid vitreopathy is generally asymptomatic. Even when the opacities are so dense that they obstruct the vision of the ocular fundus, patients do not have a reduction in visual acuity and the disease is often a fortuitous discovery during a routine eye examination.
The aetiology still remains unknown.
Sparkling synchysis
The sparkling synchysis presents clinically with multiple minute crystalline particles, shiny and coloured, suspended in a degenerated and liquefied vitreous. The appearance of these corpuscles is flat and angular, in contrast to the rounded appearance of asteroid bodies.
The crystals are mobile with the movements of the eye, but independent of the movements of the vitreous, unlike the asteroid bodies that are structurally associated with the vitreous.
During eye movements they diffuse rapidly into the vitreous cavity, but are deposited by gravity on the ocular fundus when the eye is motionless.
The sparkling synchysis is most often found in individuals under 35 years of age and occurs exclusively in severely traumatised or chronically inflamed eyes or following intravitreal haemorrhage.
Persistence of Hyperplastic Primitive Vitreous
It is a pathology that occurs in infants born at term and usually manifests itself unilaterally. This anomaly results from the lack of spontaneous regression of the fibrovascular tunic of the crystalline lens and hyalode vascularisation normally only present in the foetus. The regression phase should begin around the 2nd month of gestation to give way to the secondary vitreous.
Usually this ocular pathology is not accompanied by other systemic abnormalities. One of the main features, which shows the presence of the pathology, is a leucocoria (white pupil).
Two variants of this pathology can be recognised. The first is the Front PHPV which usually presents with microphthalmos, even of modest magnitude, and with the anterior chamber of reduced depth and possible presence of blood vessels on the iris stroma that protrude into the pupillary space or towards the lens surface.
This variant of the disease can be recognised by an important characteristic sign that consists, once the pupil has dilated, in a lengthening of the ciliary processes that adhere to the retrolenticular, contractile fibrovascular mass and pull the processes towards the centre due to the traction exerted.
The second variant of the disease, on the other hand, consists of a prominent vitreous fibrovascular cord that runs anteriorly and emerges from the optic nerve. Retinal traction folds and retinal detachments may be present in this variant.
If the pupillary foramen is not completely occluded by the opacification, remnants of hyaloid vessels can be glimpsed behind the white membrane.
Infections with bacteria, fungi and parasites
The vitreous can be infected by bacteria responsible for suppurative eye diseases (Aspergillus, Cephalosporium, Cystercus, Microfilaria, Echinococcus cysts, Toxocara canis larvae and Toxocara cati).
Age-related vitreous degeneration: myodesopsies and PVD
In the clinical field, the incidence and importance of degeneration of the vitreous gel resulting in various and in some cases disabling symptoms for patients.
The symptoms that cause the most problems are related to the vision of 'flying flies' and dark 'filaments' in the field of vision, which become even more visible in bright conditions or in the presence of light backgrounds (e.g. on a very sunny day or when standing on snow fields).
The vision of these corpuscles is the consequence of the formation of 'lumps' within the vitreous gel and the myodesopsies are nothing more than their shadow projected onto the retinal plane. The formation of vitreous thickenings is the consequence of a liquefaction of the vitreous gel due to the disruption of the mechanisms that keep the collagen fibres apart.
These fibres are physiologically enveloped by other molecules that prevent them from coming together. Should this sort of 'barrier' break down, the collagen fibres would come into contact and, due to their 'sticky' nature, aggregate to form a larger and denser network.
Once contact has occurred and the fibres have joined together, their separation is extremely difficult and intervening could even risk making the situation worse.
Through this process of aggregation of the collagen fibres, fibre-free areas would be naturally created that would change the vitreous structure, leading to a change from a gelatinous to a liquid state. Liquid areas within the vitreous cavity are referred to as 'vitreous lacunae'.
The molecules that coat collagen fibres not only prevent them from coming together, but also play another important and fundamental role. They are in fact responsible for the adhesion of the fibres to the inner limiting membrane of the retina, a very strong bond in the areas of greatest vitreo-retinal adhesion.
The passage of years, and thus the ageing of ocular tissues, causes a deterioration of the molecular lining, which, in addition to creating vitreous lacunae, can reduce the adhesion with the retinal tissue to the point of causing a Posterior Vitreous Detachment (PDV).
Vitreous liquefaction can be observed in all eyes after the age of 50, and it has been established that over the age of 80 to 90 years, more than half of the vitreous body is in a liquid state and no longer gelatinous.
Scientifically the vitreal liquefaction takes the name of synchysiswhile the formation and concentration of collagen fibres, responsible for the appearance of myodesopias, is called syneresis.
In the senile vitreous it is therefore easy for the ophthalmologist to detect both vitreous syneresis and posterior vitreous detachment, due as mentioned above to a progressive weakening and degeneration of the molecular lining.
In subjects myopesAs a result of the increased length of the eyeball, vitreous problems are generally more common than in hypermetropic or completely emmetropic eyes.
Posterior Vitreous Detachment
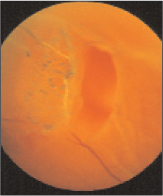
This is a rather frequent clinical condition that affects almost all eyes in old age. The loss of adhesions in the areas between the vitreous and retina in itself does not represent a pathological condition per se, but could result in serious consequences if the vitreous detaches abnormally.
The most serious complication of abnormal vitreal detachment from the retinal tissue, to which it is initially attached, is definitely the retinal rupture (Fig. 6). Retinal ruptures may be a direct consequence of a strong traction exerted by the vitreous body on the inner limiting membrane, which is 'torn' during prolapse of the vitreous within the vitreous cavity.
Patients suffering from it, as a result of the sudden separation/detachment of the vitreous from the retina, usually experience the sudden appearance of phosphenes (light signals similar to 'flashes') caused precisely by the stress exerted by the vitreous body on the retinal tissue.
An evaluation of the ocular fundus mydriasis in the presence of ocular phosphenes may detect vitreoretinal traction or an initial retinal rupture which, if properly treated, may prevent vitreoretinal complications such as retinal rupture or retinal detachment.
The persistence of vitreous traction at the retinal level can result, as already mentioned, in retinal ruptures, which in the most severe and complicated cases can turn into true Retinal Detachments with possible impairment of visual function even after retinal reattachment following surgery.
Clinically, Posterior Vitreous Detachment can be classified into:
– Partial detachment: which in turn can be subdivided according to the presence or absence of vitreo-retinal traction.
– Complete detachment: This type of Posterior Vitreous Detachment also differs according to the presence or absence of vitreous collapse anterior to the vitreous chamber. In complete vitreous detachmentIt is usually possible to appreciate Weiss's ring, which is the vitreal portion originally attached to the optic papilla. The particularity of this portion of the vitreal gel is precisely its 'ring' shape that makes it recognisable.
By means of Optical Coherence Tomography (OCT) or slit-lamp visualisation, the morphology of the vitreous body and its relationship to the underlying retinal plane can be assessed so that a detailed assessment can be made of what complications might follow.
Myodesopias: aetiology and symptoms
Commonly referred to as 'vitreous movable bodies"or 'floaters' are usually assimilated to thickenings of collagen fibres scattered in the vitreous cavity. When placed between the pupillary foramen and the retinal plane, floaters are perceived and consequently cause vision similar to the appearance of 'flying flies' or 'spider webs'.
Commonly, floaters occur during middle age and are the result of normal ageing of the vitreous structure and the scattering effect of light after the vitreous body collapses and detaches from the retinal plane.
In younger patients, however, myodesopias are usually associated with high or moderate myopia, whereas they are much rarer in emmetropic or hypermetropic patients.
The aetiology of vitreous motile bodies is thought to be sought in changes in macromolecular organisation at a young age. In young subjects, hyaluronic acid interacts with the collagen fibres to keep them sufficiently separated from each other to allow light to pass through with little or no scattering.
Should these collagen fibres come into contact and come together, the vitreous gel would lose some of its transparency, and light scattering would increase, creating diffraction effects that can disturb vision. In addition to this phenomenon, another factor contributing to the creation of vitreal opacities is the posterior detachment of the vitreous from the retinal plane, followed by its liquefaction.
It can, therefore, be said that floaters are the consequence of light scattering caused by the combination of synchysis and vitreous syneresis with posterior vitreous detachment (reported in 53% of patients over 50 years of age and in 65% of those over 65 years of age).
Posterior vitreous detachment is the first cause of the occurrence of vitreous motile bodies, followed by myopic vitreopathy, asteroid hyalosis and other systemic diseases (e.g. Marfan syndrome).
Myodesopias are reported by patients as 'lines' or 'dots' within the visual field, which become more apparent against light backgrounds or in very bright environments.

Great care must be taken should myodesopias appear because, in addition to the already mentioned fibrillar thickening, they could also be a symptom of retinal ruptures or vitreous 'bleeding'. Should these appear in association with phosphenes, an evaluation of the fundus in mydriasis should be carried out as soon as possible after the onset of symptoms.
The mobile bodies float within the vitreous cavity and move with the eye movement, casting their shadow on the retina and creating an image in the visual field.
Usually myodesopias not associated with phosphenes are a consequence of posterior vitreous detachment, while the incidence of retinal ruptures is considerably higher when they are associated with the vision of flashes of light or flashes.
Collagen fibre thickenings in the vitreous body are very difficult to treat. However, an increase in water intake and the intake of specific food supplements can lead to an improvement in symptoms due to the complete or sometimes total dissolution of the fibrillar bond.
In order to be able to better study and understand the negative effects that moving bodies have on the individual patient, it would be necessary to perform a thorough structural and functional analysis of the vitreous gel. Numerous instruments such as ultrasound, OCT, dynamic evaluation of light scattering and determination of contrast sensitivity can be used for this purpose.
Myodesopias can be the result of several causes and it is often difficult to determine the actual conditions under which this problem arises.
The main conditions in which myodesopias can develop are:
– Ageing: Vitreous deterioration, due to the passing of years, is one of the main causes of the formation of vitreous mobile bodies. It is estimated that more than 50% of people over 70 are affected by myodesopias.
– Diabetes: myodesopias, or floaters, are common in diabetic patients as the condition causes a capillary weakness that may result in small bleedings that end up floating in the vitreous gel.
– Abnormal prenatal development: Mobile bodies may sometimes be due to small cellular particles that were not completely dissolved during pre-natal development. In the last three months of gestation there is the phenomenon of regression of the hyaloid artery and, in this phase, it may happen that some particles contained in the artery remain even after its regression.
– Bulbar trauma: are one of the most common causes of floaters. Ocular trauma can, in fact, result in bulbar damage, sometimes severe, and cause the appearance of myodesopias.
– Myopia: Myopic patients, especially those with pathological myopia, have a high risk of developing myodesopias.
– Vitreitis: Vitritis are inflammations affecting the vitreous gel. Herpes, Cytomegalovirus and other viral infections are the main causes of vitritis.
– Uveitis: Inflammations of the uvea, especially the posterior ones, can be caused by infections, parasites, trauma or autoimmune diseases. In all these cases, it is very easy for vitreal mobile bodies to form.
– Vitreous anomalies: very often myodesopias can be caused by retinal ruptures or fragile capillaries.
– Cataract surgery: certain complications that may arise during cataract surgery may contribute to the formation of vitreal floaters.
Dr. Carmelo Chines
Direttore responsabile
