For Beatrice Tombolini, an ophthalmologist to be really good and prepared must be avid for knowledge, seeking to have basic skills in each subspeciality.
In 'I'll tell you a story...', the testimony of a young female doctor, Dr Beatrice Tombolini, now at the end of her specialisation course in Ophthalmology, who shares her passion and her thoughts on the importance of basic skills followed by a specialisation in a specific branch of Ophthalmology.
How did you choose your training in Ophthalmology and what is your current professional profile?

I am a final-year resident in the School of Ophthalmology directed by Prof. Francesco Bandello at the Vita-Salute San Raffaele University in Milan. A native of Sanremo, I decided to follow in my father's footsteps - my father was an ENT doctor - by enrolling in the course of Medicine and Surgery at the University of Sanremo.
The decision to become an ophthalmologist was dictated by my lifelong curiosity about the eye, a seemingly simple but in reality wonderfully complex organ. Therefore, in my fourth year of university, I approached the world of ophthalmology and never left it. The fascination of the subject was soon followed by a lively passion, which was also the result of the stimulating and avant-garde atmosphere of the Clinic and of the many teachers - of profession and of life - whom I had the honour and the good fortune to be able to follow.
I approached the different clinical and surgical subspecialties of Ophthalmology. Of each, I have tried to learn as much as possible, although I have delved more deeply into certain areas. These include: uveitis, a subject on which, with the guidance of the Prof. Miserocchi and the Dr Modorati, I developed my medical thesis; medical retina, in which I made the most of the great clinical experience of the Prof. Bandello e Querques, of the Drs. Sacconi e Cicinelliwhich also introduced me to the world of scientific research; cornea and anterior segment surgery, which I was very passionate about together with the Prof. Ferrari and to the Drs. Paganoni e Knutsson.
Can you tell us about an unusual or particularly complex clinical case that you managed to handle and solve?
I would like to share with you the clinical case of a 41-year-old woman who has been complaining of bilateral redness and photophobia for about 2 months. After an initial ophthalmic examination (in a different setting from San Raffaele), a course of topical steroid was prescribed on suspicion of conjunctivitis, with doubtful benefit. After a second episode, the patient turned to a second ophthalmologist, who sent her to our Clinic to investigate the bilateral subepithelial/stromal opacity in suspicion of corneal dystrophy.
The patient is in good general health and therefore takes no medication. She denies having any known allergies. The ocular history is silent. Her brother suffers from multiple sclerosis and associated retinal periphlebitis.
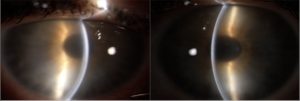 Visual acuity is 9-10/10 natural in both eyes. Biomicroscopic examination of the anterior segment shows: conjunctival hyperemia (greater in the right eye) in the absence of papillae, tarsal follicles or foreign bodies at the eversion; intact epithelium with diffuse subepithelial and stromal opacity, no endothelial deposits, large and optically empty anterior chamber, responsive pupil and transparent crystalline lens (Fig. 1).
Visual acuity is 9-10/10 natural in both eyes. Biomicroscopic examination of the anterior segment shows: conjunctival hyperemia (greater in the right eye) in the absence of papillae, tarsal follicles or foreign bodies at the eversion; intact epithelium with diffuse subepithelial and stromal opacity, no endothelial deposits, large and optically empty anterior chamber, responsive pupil and transparent crystalline lens (Fig. 1).
 The ocular pressure measured by applanation tonometry (Goldmann's) is 10 mmHg. The dilated fundoscopic examination is within normal limits. Optical coherence tomography (OCT) of the anterior segment (CSO MS-39, Italy) and in vivo confocal microscopy (IVCM) (Heidelberg, Germany) are performed. In detail, OCT shows subepithelial and stromal opacity (more evident on the right), with central corneal thickness of 605 mm and 505 mm in the right (OD) and left (OS) eye, respectively (Fig. 2).
The ocular pressure measured by applanation tonometry (Goldmann's) is 10 mmHg. The dilated fundoscopic examination is within normal limits. Optical coherence tomography (OCT) of the anterior segment (CSO MS-39, Italy) and in vivo confocal microscopy (IVCM) (Heidelberg, Germany) are performed. In detail, OCT shows subepithelial and stromal opacity (more evident on the right), with central corneal thickness of 605 mm and 505 mm in the right (OD) and left (OS) eye, respectively (Fig. 2).
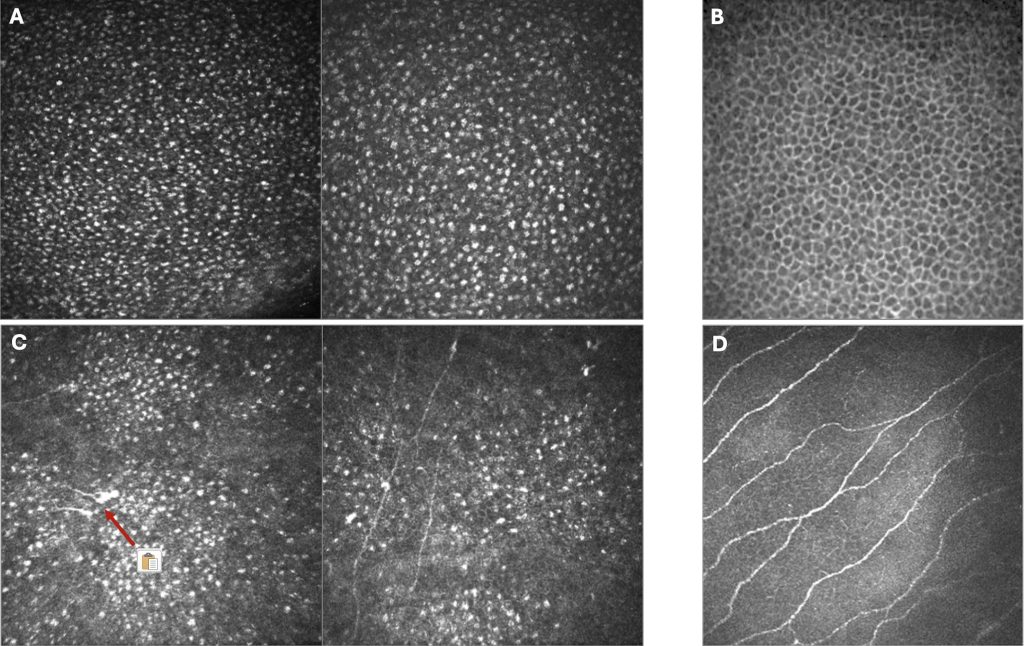
Confocal microscopy shows the following evidence: at the epithelial level diffuse hyper-reflective intracellular areas (Fig. 3A), normally absent in healthy epithelium (Fig. 3B); marked reduction of the sub-basal nerve plexus (Fig. 3C) and presence of neuromas (arrow), in comparison with a non-pathological cornea (Fig. 3D).
Later, the patient reports tingling in the distal extremities of her limbs, with subsequent electromyographic evidence of small-fibre polyneuropathy. Topical steroid therapy is administered 6 times daily on a staggered basis for 2 months in both eyes, with partial benefit. Initial diagnostic hypotheses are as follows:
- subepithelial corneal dystrophy (particularly Meesmann's, or Lisch's), although the biomicroscopic pictures under the slit lamp and confocal microscopy are clearly different;
- interstitial keratitis, for which a battery of tests was requested (TPHA and RPR, Quantiferon, serology of HSV, VZV, EBV, CMV, HIV, HBV and HCV, ANA, ANCA, rheumatoid factor, audiometric hearing test), all of which proved negative;
- paraprotein accumulation keratopathy, for which serum protein electrophoresis is prescribed, with striking evidence of a monoclonal peak in the gamma band.
The patient is referred to the haematologist. On bone marrow biopsy, atypical monoclonal restriction plasma cells (gamma/kappa chains) are observed. The result of this examination and the identification of areas of osteorefaction in CT scan lead to the diagnosis of gamma/kappa chain multiple myeloma.
Compared to the baseline (Fig. 4A), in the subsequent ophthalmic follow-ups (Fig. 4B-C) the clinical picture shows persistence of the subepithelial and stromal opacity, albeit in a less severe form, and reduced corneal thickness (OD: 507; OS: 475 mm) (Fig. 4C).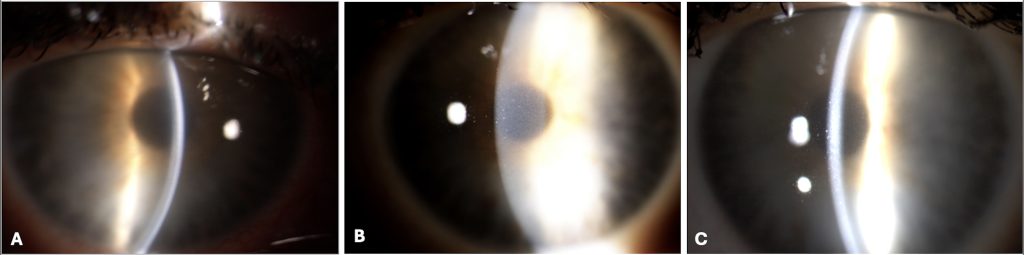
This clinical case, in my opinion, demonstrates how the ophthalmologist should not deal strictly with 'eyes', but with the patient in the broadest sense, since the eye is a window on the entire human body. In addition, the use of non-invasive diagnostic tools, such as confocal microscopy, and valuable multidisciplinary collaboration for early disease diagnosis are essential.
A few tips for your young colleagues starting out in Ophthalmology.
My advice to those who wish to approach this world is to be curious about medicine in all its aspects. Although the era of the 'all-rounders' is over, I believe that a good and well-prepared ophthalmologist should still be greedy for knowledge, seeking to have basic skills in each subspecialty. However, I believe it is equally crucial to identify an ophthalmic sub-branch in which to sub-specialise, be it medical or surgical. In this sense, I strongly encourage my younger colleagues not to desist from surgical training, as it is an integral part of our branch, as well as terribly fascinating.
My sincere good luck to everyone.
Under the heading "I tell you a story..."
- "The more I like doing something..." - Italian ophthalmologist
Interview with Dr Silvio Zagari - 'Give a woman the appropriate opportunities and...' - Italian Ophthalmologist
Interview with Dr Manuela D'Aquino - Open up to the world!!! - Italian Ophthalmologist
Interview with Dr Miguel Rechichi - Every clinical case: an opportunity for growth - Oculista Italiano
Interview with Dr Marco Zagari - The 'allologist' is a thing of the past - Oculista Italiano
Interview with Dr Francesco Cerbella - Broadening our views - Oculista Italiano
Interview with Dr Pasquale Napolitano - Let your heart lead you too - Oculista Italiano
Interview with Dr Danilo Mazzacane - The privilege of caring for people - Oculista Italiano
Interview with Dr Giovanni Scandura - "Travelling a lot to learn... - Oculista Italiano
Interview with Dr Federica Fossataro - The best refractive solution for each individual patient - Oculista Italiano
Interview Dr. Antonio Randazzo
Editorial info
Our column is open to all ophthalmologists who are interested in telling their colleagues and our web audience about a clinical case.
We invite anyone wishing to participate in our publishing project to contact
Editorial Board 'l'Oculista italiano' - Ada Puglisi
Tel. +39 095 79.22.145
E-mail: info@oculistaitaliano.it
Or write to us using one of our contact forms