A rare condition that requires timely treatment.
Eyes and ocular adnexa may be affected by what must be considered a true clinical emergency: Stevens Johnson syndrome, which must be mentioned in connection with Toxic Epidermal Necrolysis.
In the past, it was thought that they were two different diseases, but research has made it possible to understand that they are two phases of the same pathological spectrum, with Stevens Johnson syndrome being the less severe form and Toxic Epidermal Necrolysis the more extreme form.
These are rare mucocutaneous diseases, which can also be life-threatening if not managed in a timely manner.
The stages of pathology
Both are characterised by a violent rash, which rapidly spreads to the mucous membranes and results in epidermal vesicles, necrosis and flaking of the epidermis.
Skin involvement is preceded in most cases by a prodromal stage with symptoms such as fever, malaise, sore throat and cough.
Skin lesions: prevalence
According to a commonly accepted classification, mucocutaneous changes affect 30% in toxic epidermal necrolysis; involvement between 10 and 30% of the body surface is considered an overlap between Stevens-Johnson syndrome and toxic epidermal necrolysis.
Aetiology
The trigger is usually an autoimmune reaction of hypersensitivity to drugs or, more rarely, an infection.
The drugs were found to be responsible for approximately 50% of Stevens-Johnson syndrome cases and up to 95% of toxic epidermal necrolysis cases.
The drugs responsible
The drugs most frequently involved are:
- Sulphonamides (e.g. sulfasalazine)
- Other antibiotics (e.g. aminopenicillins - usually ampicillin or amoxicillin, fluoroquinolones, cephalosporins) - Anti-convulsant drugs (e.g. phenytoin, carbamazepine, phenobarbital, valproate and its derivatives, lamotrigine)
- NSAIDs (e.g. piroxicam, meloxicam)
- Antiretroviral drugs (e.g. nevirapine)
- Other drugs (e.g. allopurinol, chlormezanone)
The non-drug cases are attributed to:
- Infections (mostly from Mycoplasma pneumoniae)
- Vaccination
- Graft-versus-host disease (GVHD)
Treatment
To counteract the disease, in the case of a drug reaction, the drug responsible must be identified and discontinued.
Symptomatic and supportive therapy should also be used, based on cyclosporine, plasmapheresis or intravenous immunoglobulins, and possibly early corticosteroid therapy idioms and TNF-alpha inhibitors.
idioms and TNF-alpha inhibitors.
Mortality can be as high as 7.5% in children, who still react better than adults, and 20-25% in adults, but tends to be lower with early treatment.
Eye symptoms
In the acute skin involvement phase, the following have been reported acute ocular symptoms in 27-80% of patients and the most frequently affected ocular tissue was the conjunctiva (90%).
İthe level of severity ranges from conjunctival hyperemia to complete epithelial degeneration of the ocular surface.
A timely check-up by an ophthalmologist is essential to prevent long-term eye sequelae.
Eye treatment
Specific aspects of ocular treatment include the removal of mucus and crusts during the acute phase to ensure appropriate ocular hygiene in the first place.
Topical steroid treatment
Controlled studies have also shown that early topical steroid treatment (started within the first week) is effective in preventing chronic corneal complications and leads to better visual outcomes.
It is therefore recommended that in patients with Stevens Johnson syndrome who have damage to the corneal epithelium, topical steroid therapy should be continued, adapted according to the patient's clinical condition, and, if necessary, combined with the use of a corneal contact lens bandage.
Complications
Although the therapy may be effective, late complications may occur in some patients.
Daily massage of the fornix (with a fornix spatula) is recommended to prevent the possible development of simblefaron during the acute phase.
In recent years, the use of a simblefaron ring has also been used in paediatric patients.
Tear duct occlusion is an intervention that is considered to manage cases of severe dry eye.
Resolution
With appropriate treatment, skin lesions in patients with Stevens Johnson syndrome typically regress within a few weeks.
However, the relapse rate is high, with one third of patients relapsing. This underlines, once again, the need for long-term follow-up of these patients.
Conclusions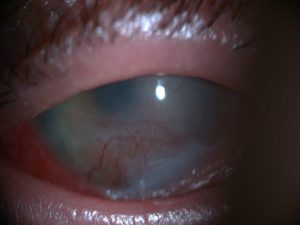
Recent studies have emphasised the need to consider the risk of SJS and TEN in patients using a variety of drugs, although drug reactions are less common in children than in adults.
Early diagnosis of the disease and immediate withdrawal of the responsible drug are crucial to reduce mortality and morbidity.
Consensus
At present there is no consensus on the best treatment for toxic epidermal necrolysis and Stevens Johnson syndrome.
The basis of treatment for this syndrome is supportive and symptomatic therapy. Treatment directed against the causative agent may involve the addition of systemic steroids, intravenous immunoglobulins (IVIg), immunosuppressive drugs, haemodialysis and plasmapheresis.
It is widely accepted that systemic steroid therapy (1-2 mg/kg/day, for 3-5 days, intravenous immunoglobulins or oral prednisolone) administered in the early stages of the disease inhibit immunological mechanisms and facilitate disease control.
- Duong T.A., Valeyrie-Allanore L., Wolkenstein P., Chosidow O. Severe cutaneous adverse reactions to drugs. Lancet. 2017;390:1996-2011. doi: 10.1016/S0140-6736(16)30378-6.
- Frey N., Jossi J., Bodmer M., Bircher A., Jick S., Meier C.R., Spoendlin J. The Epidemiology of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in the UK. J. Investig. Dermatol. 2017;137:1240-1247. doi: 10.1016/j.jid.2017.01.031.
- Alerhand S., Cassella C., Koyfman A. Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in the Paediatric Population: A Review. Pediatric Emerg. Care. 2016;32:472-478. doi: 10.1097/PEC.0000000000000840.
- Garcia-Doval I., LeCleach L., Bocquet H., Otero X.L., Roujeau J.C. Toxic epidermal necrolysis and Stevens-Johnson syndrome: Does early withdrawal of causative drugs decrease the risk of death? Arch. Dermatol. 2000;136:323-327. doi: 10.1001/archderm.136.3.323.
- Sotozono C, Ueta M, Koizumi N, Inatomi T, Shirakata Y, Ikezawa Z, et al. Diagnosis and treatment of Stevens-Johnson syndrome and toxic epidermal necrolysis with ocular complications. Ophthalmology 2009;116(4):685-90.
- Van Zyl L, Carrara H, Lecuona K. Prevalence of chronic ocular complications in stevens johnson syndrome and toxic epidermal necrolysis. Middle East Afr J Ophthalmol 2014; 21(4):332-5.
