Shingles infection
Ophthalmic herpes zoster infection is so common because the virus, which is the same one responsible for the childhood chickenpoxOnce contracted, it remains latent in the nerve cell bodies, without causing any symptoms.
Years or decades after a chickenpox infection, the virus can spread from one or more ganglia along the nerves of an affected segment and infect the corresponding dermatomere (an area of skin served by a spinal nerve), causing a painful rash.
Herpetic pain
The immune system under normal conditions is able to suppress the reactivation of the virus and prevent the reactivation of the herpetic infection, which is not the case in immuno-depressed patients and the elderly.
The severity of the ocular clinical picture and the fact that herpetic disease is not a 'single-stage' disease, but rather a recurring infection can also lead to the chronicisation of the post-neuralgia pain.
This makes it relevant for ophthalmologists and health authorities to promote the vaccination of populations against the zoster virus.
The vaccine use would, therefore, be especially desirable in these cases for a number of concomitant reasons. Firstly, throughout the developed world, there has been a progressive lengthening of average life expectancy and, therefore, an increase in the elderly component of the population, which is more likely to experience herpetic infection.
Secondly, the elderly tend to be more susceptible to zoster infection due to a number of age-related conditions such as immuno-senescence, to which can be added possible immuno-suppression from pharmacotherapy or diseases that compromise the immune system.
Pain control
Effective pain control in the case of ophthalmic herpes zoster infection, which can involve the cornea, is essential, first and foremost to alleviate clinical manifestations, but above all it is crucial to reduce the risk of developing the dreaded postherpetic neuralgia.
Neuro-modulation
Recently, neuro-modulation therapy, which is also increasingly being applied in the treatment of systemic shingles pain, has been put forward as an option for the management of neuropathic pain in the ocular region, especially in the forehead.
A key factor in the success of neuro-modulation therapy is the targeting of damaged nerve fibres. In particular, a clinical study on a new neuro-modulation strategy for the management of ophthalmic herpes zoster pain, targeting both the peripheral branch and the trigeminal ganglion, has recently been completed.
The onset of pathology
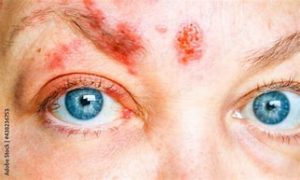 Ophthalmic herpes zoster (HZO) is caused, as mentioned above, by the reactivation of the latent varicella-zoster virus and typically results in a painful eruption with blisters in the area corresponding to the ophthalmic branch of the trigeminal nerve, also affecting the eyes.
Ophthalmic herpes zoster (HZO) is caused, as mentioned above, by the reactivation of the latent varicella-zoster virus and typically results in a painful eruption with blisters in the area corresponding to the ophthalmic branch of the trigeminal nerve, also affecting the eyes.
It is estimated that ophthalmic herpes constitutes approximately 10-20% of the total herpetic infections.
Risk factors
Risk factors for the development of this infection, which can also involve the nose, include:
- advanced age
- conditions of immuno-compromise
- the presence of comorbidities.
A number of studies have recently been published that also report experimental evidence of a potential causal correlation between ophthalmic herpes zoster and vaccination against COVID-19, which can lead to the onset of a viral infection that can also affect the eye.
Symptoms
A characteristic manifestation of ophthalmic herpes zoster is intense pain in the eye, characterised by a stabbing pain that also radiates to the periocular area and localised pain in the acute phase of the vesicular eruption.
Approximately half of all patients with ophthalmic herpes zoster may develop postherpetic neuralgia with ophthalmic involvement. This condition is characterised by moderate to severe facial pain that may persist for more than 3 months after the onset of the skin lesion.
Specific features of this neuropathy are the presence of a continuous, spontaneous burning pain with electric shock-like twinges in a paroxysmal phase, allodynia (Ed: painful impulse felt by the person following an innocuous stimulus) and hyperalgesia (Ed: increased response to a stimulus capable of provoking painful sensations).
The quality of life in these patients is therefore particularly compromised and it is therefore necessary to find strategies that can alleviate the painful symptoms.
Treatment
In the management of herpes zoster infection, especially in advanced age, first-line treatment involves the oral administration of acyclovir or systemic antiviral analogues from the early stages of infection, although the ability of these drugs to reduce the risk of postherpetic neuropathy remains controversial.
In addition to antiviral treatment, it is essential to administer specific pain relief therapy, most often with analgesic drugs, including tricyclic antidepressants, antiepileptics, opioids and topical analgesics.
If oral therapy proves insufficient, surgical treatments, such as temporary blockade of local nerve sensitivity to provide immediate short-term pain relief, may also be considered.
What's new in neuro-modulation
In a recent study, Dual-neuromodulation strategy in pain management of herpes zoster ophthalmicus: retrospective cohort study and literature review - PubMed (nih.gov) neuro-modulation therapy was tested by implanting an electrical stimulator of the supraorbital and supratrochlear nerve plexuses, capable of delivering continuous stimulation to cover the areas affected by pain. However, 22.2% of patients with HZO also experience pain in the irradiation area of the second branch of the trigeminal nerve (i.e. the maxillary nerve), which cannot be reached by peripheral ophthalmic stimulation. In very severe cases, patients with HZO may have pain involving all three branches of the trigeminal nerve. Therefore, a dual neuro-modulation strategy has been investigated, which simultaneously targets the peripheral nerve branch and Gasser's ganglion by combining short-term continuous peripheral nerve stimulation (PNS) with pulsed radiofrequency (PRF) of the trigeminal ganglion
The primary outcome, which may include the presence of vesicles, was measured in terms of pain intensity before and after neuro-modulation therapy, as measured by the Visual Analogue Scale (VAS)
The VAS scale is one of the best known one-dimensional outcome measures for measuring pain intensity. It corresponds to the visual representation of the extent of pain felt by the patient and consists of a predetermined line 10 cm long, where the left end corresponds to 'no pain' and the right end to 'worst possible pain'. The patient is asked to draw a mark on the line representing the level of pain experienced.
Results
The results show that the dual neuro-modulation strategy is able to ensure superior results in terms of the persistence of the analgesic effect of the therapy, compared to continuous peripheral nerve stimulation alone, which is also very important in view of the fact that herpetic ophthalmic infection tends to be relapsing.
On the subject of herpes virus eye infections see also:
- Current and emerging therapies for herpes simplex eye infections - Oculista Italiano
- Neuropathy after shingles infection: if and when to vaccinate - (oculistaitaliano.it)
- Ma J, Wan Y, Yang L, Huang D, Zhou H. Dual-neuromodulation strategy in pain management of herpes zoster ophthalmicus: retrospective cohort study and literature review. Ann Med. 2023;55(2):2288826. doi: 10.1080/07853890.2023.2288826. Epub 2023 Dec 4. PMID: 38048401; PMCID: PMC10836271.
- Rallis KI, Fausto R, Ting DSJ, et al. Manifestation of herpetic eye disease after COVID-19 vaccine: a UK case series. Ocul Immunol Inflamm. 2022;30(5):1136-1141. doi: 10.1080/09273948.2022.2046795.
- You IC, Ahn M, Cho NC. A case report of herpes zoster ophthalmicus and meningitis after COVID-19 vaccination. J Korean Med Sci. 2022;37(20):e165. doi: 10.3346/jkms.2022.37.e165.
- Martora F, Fabbrocini G, Picone V. A case of herpes zoster ophthalmicus after third dose of comirnaty (BNT162b2 mRNA) vaccine. Dermatol Ther. 2022;35(5):e15411.
