The risks that prolonged and inappropriate use of anaesthetic eye drops can pose for the cornea and the entire ocular surface.
Very often, patients with eye disorders go to the ophthalmologist or general practitioner complaining of pain as their main symptom, a pain that, especially if related to a disease or injury of the cornea, can be very acute and debilitating.
The patient therefore needs treatment to counteract the pain sensation and, in parallel, specific therapy to eliminate the underlying cause.
Eye drops containing anaesthetics are a remedy against pain, but care must be taken as their excessive or prolonged use can lead to serious damage to the ocular surface as a whole and to the cornea in particular.
Abuse of topical anaesthetics is, in fact, one of the most frequent forms of self-induced ocular damage. In most cases, this is iatrogenic damage, i.e. caused by the misuse or overuse of one or more drugs, some of which are prescribed by ophthalmologists, optometrists, general practitioners and emergency physicians to counteract ocular pain.
The most commonly used topical anaesthetics are tetracaine, lidocaine, proparacaine and oxybuprocaine.
Potential risk situations are manifold and include:
- the development of a real addiction to drugs that relieve or eliminate pain
- easy access to topical anaesthetics, especially when available as over-the-counter products
- the presence of neurological pathologies
- the prescription of topical anaesthetics after refractive surgery or corneal transplantation.
Local effects on the corneal surface
The damaging effects on the cornea are related to the ability of anaesthetic agents to inhibit the intrinsic characteristic of corneal epithelial cells to migrate and divide, damaging vinculin and actin filaments. Morphological changes visible under the electron microscope include loss of microvilli, anaesthetic deposits on microvilli and/or cell membranes and increased desquamation.
In addition, preservatives contained in some topical anaesthetics, such as benzalkonium chloride, may lead to toxic effects on the ocular surface.
Clinical aspects
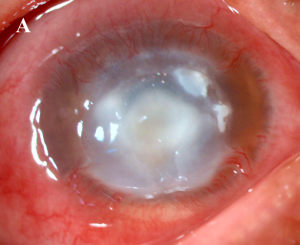 The first clinical sign is usually an erosion of the corneal epithelium, while the stroma is not yet involved. If the abuse of topical anaesthetics is persistent, epithelial erosions are associated with conjunctival hyperemia, stromal oedema, stromal infiltrates (the classic ring infiltrates), folds in Descemet's membrane, endothelial damage and ocular inflammation with possible hypopion. Corneal damage, if severe and persistent, can endanger vision and lead to the need for penetrating keratoplasty.
The first clinical sign is usually an erosion of the corneal epithelium, while the stroma is not yet involved. If the abuse of topical anaesthetics is persistent, epithelial erosions are associated with conjunctival hyperemia, stromal oedema, stromal infiltrates (the classic ring infiltrates), folds in Descemet's membrane, endothelial damage and ocular inflammation with possible hypopion. Corneal damage, if severe and persistent, can endanger vision and lead to the need for penetrating keratoplasty.
Diagnosis
An early diagnosis of the abuse of topical anaesthetics is certainly the most important condition for ensuring a better visual outcome. It is very important that, in the presence of a suspicious clinical picture, the ophthalmologist or family doctor carefully examines all possible hypotheses.
Very often, corneal erosions from abuse of topical anaesthetics are confused with manifestations of other serious corneal infections, so differential diagnosis is important with conditions such as Acantamoeba keratitis, herpetic keratitis, fungal keratitis and bacterial keratitis.
Management
It is of primary importance to immediately discontinue the use of topical anaesthetics and any other eye drops to which toxic effects on the ocular surface may be attributed.
Alternative pharmacological approaches with oral analgesics and/or regional anaesthesia (peribulbar, retrobulbar, injections below Tenon's capsule) must be used to contain the pain.
It may be necessary to hospitalise the patient and he or she may need to undergo a neurological examination, while it is best to avoid topical steroid medication, which could lead to further thinning of the cornea.
Finally, a key element for a primary prevention strategy is an educational course that makes doctors, ophthalmologists, optometrists and pharmacists aware of the potential toxicity of topical anaesthetics and the risks of their misuse by patients.
- Fraser R, Walland M, Chan E, Crock C. Topical anaesthetic in the treatment of corneal epithelial defects: What are the risks? Aust J Gen Pract. 2019 Aug;48(8):504-506. doi: 10.31128/AJGP-09-18-4709. PMID: 31370122.
- McGee H, Fraunfelder F. Toxicities of topical ophthalmic anaesthetics. Expert Opin Drug Safe 2007;6(6):637-40
- Rosenwasser GO, Holland S, Pflugfelder SC, et al. Topical anaesthetic abuse. Ophthalmology 1990; 97: 967-975.
- Risco JM, Millar LC. Ultrastructural alterations in the endothelium in a patient with topical anaesthetic abuse keratopathy. Ophthalmology. 1992;99(4):629-633.
